Health Blog | 3 MIN READ
Temporomandibular Joint (TMJ) Disorders
Dr. Alaa
Overview
Temporomandibular Joint and Muscle Disorders are groups of conditions that cause pain and dysfunction in the jaw joints and the surrounding muscles. Research suggests that over 10 million Americans suffer from TMJ, which is found more in women. For the vast majority, the pain comes in occasional cycles. People also may develop long-term symptoms.
If you have questions about TMJ, you’re not alone! TMJ specialists are constantly searching for new answers as to what causes these disorders and what treats them.
Understand The Anatomy Of Your Jaw Joints :
The temporomandibular joint connects the mandible (lower jaw) to the temporal bone (side of the head). Because these joints are flexible and can comfortably move up and down and side to side, allowing us to chew, speak or yawn. You can feel it by placing your hand right in front of your ear and opening and closing your mouth.
Classified TMJ disorders :
■ Arthritis or Rheumatoid Arthritis, is a group of inflammatory joint disorders that affect the temporomandibular joint.
■ Myofascial Pain, discomfort in muscles that control jaw function
■ Internal Dearraged Joints, a displaced disc, dislocated jaw, or injured condyle.
Patients may have one or more conditions at the same time. Other conditions that may or may not be correlated can co-exist
TMJ disorder is a joint connecting your jawbone to your skull
Common Symptoms And Causes?
Trauma or prolonged stress to the jaw may result in or play a role in TMJ disorders; scientists are yet to find a direct cause as it is more common in women, they are exploring the link between female hormones and TMJ disorders.
A variety of signs may indicate TMJ disorders. Particularly pain in the muscles responsible for chewing or discomfort in the joints, other common symptoms include:
■ Jaw Muscle Stiffness
■ Limit In Range Of Movement
■ Locking Of The Jaw
■ Painful Clicking Or Popping In The Jaw Joint When Opening Or Closing The Mouth
■ Changes In The Way The Upper And The Lower Teeth Fit
How Does One Get Diagnosed?
Identifying and diagnosing may sometimes be confusing as there are no exact causes set. A physiotherapist TMJ specialist will take note of your symptoms along with taking a look at the patient’s detailed medical and dental history and an examination of the neck, face, jaw, and head. Imaging studied may be required.
Treatment

Experts suggest conservative, reversible treatments more than surgery that do not invade the tissue of the jaw, face, or joint and do not result in permanent changes.
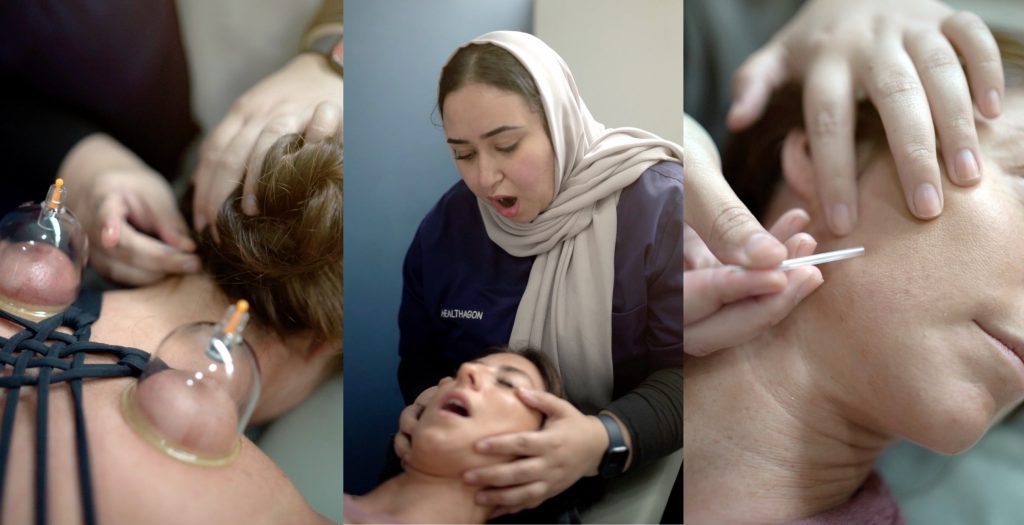
Dry needling is an excellent option to spot-treat the jaw muscles and can immensely decrease pain, inactivate trigger points, restore function, increase range of motion and overall treat muscle tissue.
It can target and release muscle, a thin microfilament needle can change myofascial restrictions by inducing a twitch response in the muscle. This twitch response is associated with enhanced flexibility and blood circulation, ultimately reducing pain.
You may feel a slight discomfort at the moment, but instant relief after the session. The initial soreness wears off very quickly.
Ultrasound is a therapeutic application that promotes tissue healing via tissue regeneration and repair. Using deep heat provides relief, relaxation speeds recovery, and resolves inflammation common in TMJ disorders.
Self-remedies :
■ Opt for soft foods
■ Ice Therapy
■ No extreme jaw movements (loud singing, wide yawning, and gum chewing)
■ Stretching and Strengthing Exercise to increase range of motion and reduce stress
Facial and Jaw Exercises :
Goldfish exercise
Mandibular Stabilization Exercise
Cervical Retraction “Chin Tucks”
Side-to-Side Jaw Exercise
Tongue Up Exercise









1 thought on “Temporomandibular Joint (TMJ) Disorders”
Best article ever